
- Home >
Resources


ACTIVATE: ¿Qué es Salud Digital?
Ahora puede ver ACTIVATE en acción a través de breves videos creados por nuestros compañeros Diverse Health Hub. ¿Qué es la salud digital? presenta a una madre ocupada con poco tiempo extra para cuidar de su propia salud, y muestra cómo ACTIVATE puede ayudar.
Research Areas & Topics: Health, Technology, Digital Health, ACTIVATE

ACTIVATE: What is Digital Health?
Now you can see ACTIVATE in action through brief videos created by our partners Diverse Health Hub. What Is Digital Health? introduces a busy mom with little extra time or bandwidth to take care of her own health and shows how ACTIVATE can help.
Research Areas & Topics: Health, Technology, Digital Health, ACTIVATE

Introducing ACTIVATE
Now you can see ACTIVATE in action through brief videos created by our partners Diverse Health Hub. In Introducing ACTIVATE, follow a patient as he discovers how ACTIVATE can help him learn about his chronic conditions (diabetes and high blood pressure) and connect with his health care team.
Research Areas & Topics: Telehealth, Health, ACTIVATE

Introducing Livingston Community Health Center’s ACTIVATE program
ACTIVATE is a demonstration project using digital health to improve the health and well-being of rural or underserved communities in partnership with community health centers. ACTIVATE is designed to help patients learn more about their diabetes and/or high blood pressure and how to help get them under control, all from the comfort of their own home!
Research Areas & Topics: Telehealth, Health, ACTIVATE

Lessons on Scaling Equitable Vaccine Distribution to Help High-Risk Populations
A conversation with Dr. David Lindeman, Director of CITRIS Health; Veronica Chavez, Community Outreach Manager at Livingston Community Health; Helidee Millan-Govea, Community Outreach Manager at Livingston Community Health; Sheri Peifer, Senior VP and Chief Strategy Officer of Eskaton, Darlene Cullivan, Senior Manager of Outreach and Impact at Eskaton and Dr. Sheri Belafsky, Medical Director of Healthy Davis Together, as they discuss the lessons learned through the development and deployment of their vaccine initiatives, the importance of partnerships with trusted community organizations, and the equity considerations required for building an equitable infrastructure for providing vaccines to underserved populations.
Research Areas & Topics: Telehealth, ACTIVATE, Lighthouse

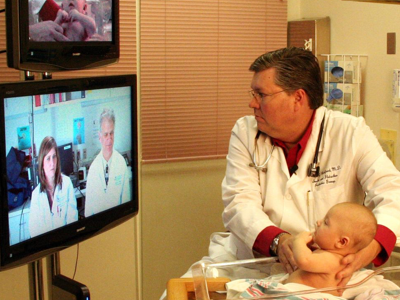
Personalized Telehealth in the Future: A Global Research Agenda
As telehealth plays an even greater role in global health care delivery, it will be increasingly important to develop a strong evidence base of successful, innovative telehealth solutions that can lead to scalable and sustainable telehealth programs. This paper has two aims: (1) to describe the challenges of promoting telehealth implementation to advance adoption and (2) to present a global research agenda for personalized telehealth within chronic disease management. Using evidence from the United States and the European Union, this paper provides a global overview of the current state of telehealth services and benefits, presents fundamental principles that must be addressed to advance the status quo, and provides a framework for current and future research initiatives within telehealth for personalized care, treatment, and prevention. In this paper, the members of the Transatlantic Telehealth Research Network offer a 12-point research agenda for future telehealth applications within chronic disease management.
Research Areas & Topics: Telehealth, TTRN

Presentamos ACTIVATE
Ahora puede ver ACTIVATE en acción a través de breves videos creados por nuestros compañeros Diverse Health Hub. En Presentamos ACTIVATE, siga a un paciente mientras descubre cómo ACTIVATE puede ayudarlo a aprender sobre sus condiciones crónicas (diabetes y presión arterial alta) y conectarse con su equipo de atención médica.
Research Areas & Topics: Telehealth, Health, ACTIVATE
